Weight loss surgery, also known as bariatric surgery, has become an increasingly popular option for individuals struggling with obesity. It offers the promise of significant weight loss and improved health. However, like any medical procedure, weight loss surgery is not without its potential complications. One such complication that has gained attention is the development of ulcers.
In this comprehensive blog post, we will delve into the world of weight loss surgery and ulcers. We’ll explore the types of weight loss surgeries, their benefits, and the risk of ulcers associated with them. Additionally, we will discuss the causes, symptoms, and management of ulcers in individuals who have undergone weight loss surgery.
Before we can understand the connection between weight loss surgery and ulcers, it’s crucial to have a clear understanding of the various types of bariatric procedures. The three most common weight loss surgeries are:
Gastric Bypass Surgery (Roux-en-Y): This procedure involves creating a small pouch at the top of the stomach and rerouting the small intestine to this pouch. This restricts the amount of food a person can eat and reduces calorie absorption.
Sleeve Gastrectomy: During this surgery, a significant portion of the stomach is removed, leaving a banana-shaped sleeve. This reduces the stomach’s capacity and results in less calorie intake.
Adjustable Gastric Banding (Lap-Band): In this procedure, an inflatable band is placed around the upper part of the stomach, creating a small pouch. The band can be adjusted to control food intake.
Weight loss surgery is not only about shedding excess pounds; it also offers numerous health benefits. Some of the positive outcomes of these procedures include:
Significant Weight Loss: Bariatric surgery can lead to substantial weight loss, which is often difficult to achieve through diet and exercise alone.
Improved Metabolism: Weight loss surgery can enhance insulin sensitivity and help manage conditions like type 2 diabetes.
Resolution of Obesity-Related Health Issues: Many patients experience a reduction or resolution of conditions such as sleep apnea, high blood pressure, and high cholesterol after weight loss surgery.
Enhanced Quality of Life: With improved health and self-esteem, patients often report a better quality of life after their surgery.
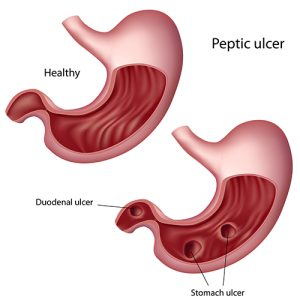
While weight loss surgery offers significant benefits, it can also increase the risk of developing peptic ulcers. Peptic ulcers are open sores that develop on the inner lining of the stomach or the upper part of the small intestine. The following factors contribute to the development of ulcers post-bariatric surgery:
Changes in Stomach Acidity: After surgery, the stomach’s acid production may increase, leading to an environment where ulcers are more likely to form.
Medications: Many patients receive nonsteroidal anti-inflammatory drugs (NSAIDs) to manage postoperative pain. NSAIDs can irritate the stomach lining and contribute to ulcer development.
Smoking: Smoking is a known risk factor, and many individuals who undergo weight loss surgery continue to smoke.

It is important to recognize the symptoms after weight loss surgery to ensure timely diagnosis and treatment:
Abdominal Pain: A burning or gnawing pain in the abdomen, usually in the upper part, is a typical symptom of ulcers.
Nausea and Vomiting: Some individuals may experience nausea and vomiting, which can be persistent.
Loss of Appetite: A diminished appetite is another common sign of ulcers.
Weight Loss: Unintended weight loss may occur due to discomfort and a reduced appetite.
Dark Stool or Vomit: If an ulcer is bleeding, it can lead to the passage of dark, tarry stools or bloody vomit.
Once ulcers are diagnosed, effective management is essential. Here are some strategies for managing ulcers in individuals who have undergone weight loss surgery:
Medications: Proton pump inhibitors (PPIs) and H2 blockers are commonly prescribed to reduce stomach acid and promote ulcer healing.
Lifestyle Modifications: Patients are advised to quit smoking and avoid alcohol. They should also steer clear of NSAIDs.
Dietary Adjustments: A diet that includes soft, non-irritating foods can help ease discomfort during the healing process.
Follow-Up Care: Regular follow-up appointments with healthcare providers are crucial to monitor ulcer healing and ensure proper treatment.
Surgical Intervention: In rare cases, surgery may be necessary to treat complications of ulcers, such as perforation or bleeding.
Weight loss surgery has proven to be an effective option for individuals battling obesity, offering numerous benefits for improved health and quality of life. However, it’s essential to be aware of potential complications such as peptic ulcers. Understanding the causes, symptoms, and management of ulcers after weight loss surgery is crucial for the long-term success of the procedure.
Patients should maintain open communication with their healthcare providers, follow their recommendations, and make necessary lifestyle changes to reduce the risk of developing ulcers. With proper care and attention, the potential risks can be minimized, allowing individuals to enjoy the full benefits of their weight loss surgery.
Remember that this blog provides general information and is not a substitute for professional medical advice. If you or someone you know is considering weight loss surgery or is experiencing symptoms of ulcers, it is essential to consult with a healthcare professional for personalized guidance and care.
Don’t forget to follow us in all our social media.
– Youtube
– Instagram
– Tiktok
We will provide you with immediate follow-up!
In order to offer you the method that best suits your needs, it is crucial for us to have knowledge of your medical history.
Please complete the following detailed health questionnaire with as much information as possible.
This will help us get to know you better.
©2023 Dr. Luis Pasten | Overweight Reduction Center | All Rights Reserved.