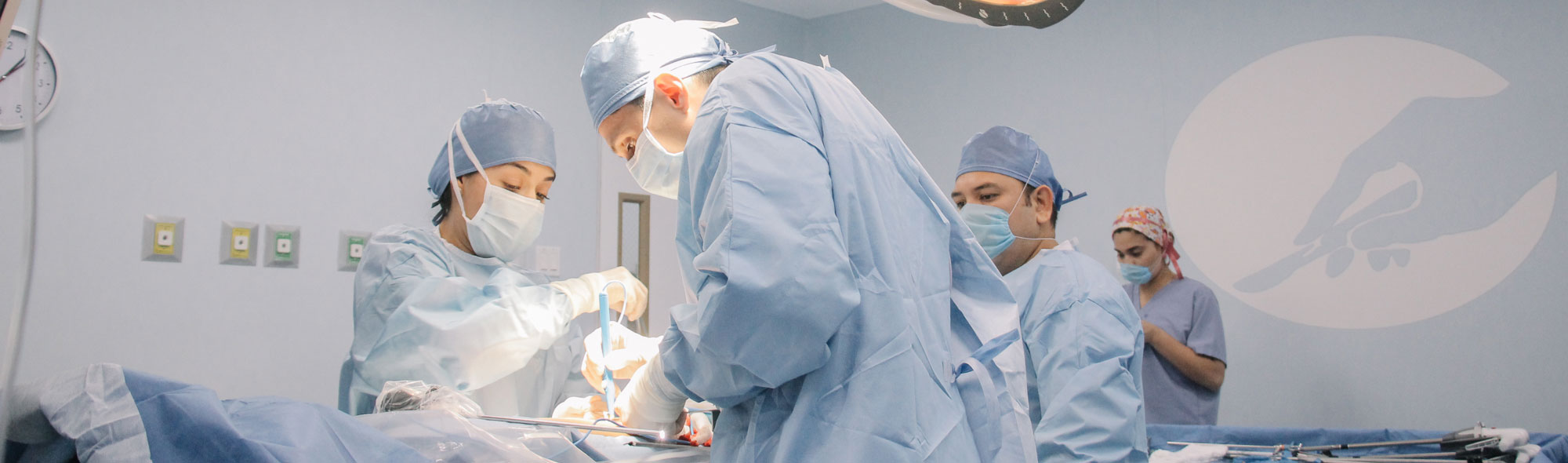
Harmony on the Journey: The Crucial Role of Partner Support in a Gastric Sleeve Patient’s Transformation
Gastric Sleeve Patient’s Partner Embarking on a journey toward health and wellness is a profound and personal endeavor. For individuals undergoing gastric sleeve surgery, the decision marks a transformative chapter [...]





